July/August 2018
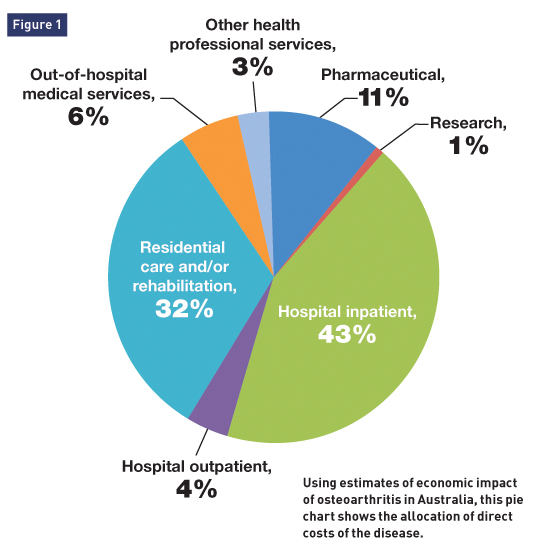
Knee Osteoarthritis in Older Adults: A Nonsurgical, Regenerative Approach to Pain Relief A new strategy recruits stem cells to enhance the body's normal healing process. Osteoarthritis (OA), the most common type of arthritis, affects more than 30 million adults in the United States, with the highest prevalence reported in those ages 65 and older.1 OA negatively affects patients with respect to diminished quality of life, including limited physical function, a reduced ability to perform daily tasks, and pain with activities of daily living.2 Patients suffering from OA also are at increased risk of falls (more than 2.5 times greater risk for two or more significant falls).3 Falls in this patient population can result in substantial injury and fractures when compared with adults without arthritis.3 As described by Nick Willett, PhD; Robert Guldberg, PhD; and their colleagues at the Georgia Institute of Technology, OA is a degenerative joint disease that's the leading cause of chronic disability in the United States.4 OA is a chronic, progressive degeneration of the articular cartilage accompanied by cartilage loss, joint deformity, pain, and instability. At its end stage, OA often results in exposure of bone surfaces, which results in progressive pain, loss of function of the affected joint, and disability. General features of OA include globalized joint pain, swelling, stiffness, joint tenderness, locking, and significant loss of motion. Current treatment modalities target the symptomatic management of OA, which may ultimately include surgical procedures such as joint replacement for severely symptomatic patients or those who fail conservative measures. During these surgical procedures, the degenerated joint is surgically replaced (ie, hip, knee, and shoulder arthroplasty), which generally restores motion and substantially reduces pain. OA can be severely disabling and has been reported to be the single most expensive condition among Medicare patients.5 There are a variety of causes postulated for arthritic conditions, among them hereditary factors, including increased commonality among twins and siblings. Additional etiologies include congenital or pathological joint stress, excess body weight, muscle weakness, rheumatologic conditions, and traumatic injuries to a joint. OA is a leading cause of disability among older adults, affecting upwards of one in eight people. The impact of this highly prevalent disease not only on individuals but also on society is quite formidable. Societal trends, including aging of the population, obesity prevalence, and traumatic joint injury indicate that this disease is expected to increase in incidence by about 50% over the next 20 years. According to a Morbidity and Mortality Weekly Report (MMWR) from November 2013, based on a National Health Interview Survey performed by the Centers for Disease Control and Prevention (CDC) in Atlanta, 52.5 million (22.7%) adults older than 18 had self-reported doctor-diagnosed arthritis, while 22.7 million (9.8%, or 43.2% of those with arthritis) reported arthritis-attributable activity limitation.3 The MMWR paper indicates that the recent figures cited by the CDC were consistent with an earlier projection of 55.7 million adults with arthritis by 2015 and 67 million by 2030.3 The authors conclude that arthritis and resulting activity limitations create a substantial personal and societal disease burden in the United States, with prevalence exceptionally high in those who are unable to work, disabled, and in fair to poor health, even when adjusted for age.3 Symptomatic and advanced knee OA is particularly impactful on overall health and mobility. The overall prevalence of symptomatic knee OA was 15.6 million, with 8.9 million having advanced OA.6 The costs associated with knee OA are significant. For example, a recent review of 94 articles addressing this issue showed that the average US direct costs—that is, doctor and related costs from medical care for knee OA—ranged from $1,442 to $21,335, while costs from lost wages and productivity ranged from $238 to $29,935.7 From 2002 to 2012, the number of individuals in the United States with a total knee replacement doubled from 2 million to 4 million.8 The bulk of hospital admissions for OA involve total joint replacement surgeries, with an estimated cost in 2008 (when the estimate was over 1 million annual procedures, not the 4 million of today) of $15 billion in total health care expenditures.8 Older adults opting for knee replacement are likely to suffer longer hospital stays and higher risks of both ICU admission and postoperative complications as compared with younger patients.9 Representative OA cost data are shown in Figure 1 from a recently published article by Australian researchers.8
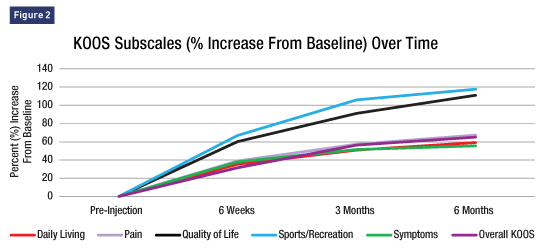
As a result of patient preference and/or medical comorbidities and costs, health care providers need to be prepared to care for and counsel all patients suffering from knee OA who are looking for nonsurgical alternatives. Existing nonsurgical treatment options for OA include physical therapy, activity modification, bracing, and drug therapy. Medications including NSAIDs such as ibuprofen and arthritis-strength acetaminophen are common first-line modalities. In addition, approved injectable treatments such as corticosteroids or hyaluronic acid-based treatments are also commonly employed. Each of these options either has limited effectiveness or is associated with potentially adverse complications. For example, NSAID use is limited by its impact on cardiovascular, gastrointestinal, and renal systems, as well as its interaction with other medications a patient may take. Other less well studied approaches include knee injections with a patient's own bone marrow cells, patient-derived platelet rich plasma solutions, and stem cell injections. Each of these involves an invasive procedure (bone marrow or fat aspiration, needle stick), and thus far no consistent data have been delineated to indicate to what extent these approaches are safe and effective in treating knee OA. Use of these various interventions, now being labeled "regenerative" approaches, represents attempts by physicians to use products that offer more than symptomatic relief to OA patients. Clinical trials over many years have tested drugs with so-called disease-modifying potential in OA (DMOADs), including matrix-metalloproteinase inhibitors, cytokine blockers, inhibitors of inducible nitric oxide synthase, and doxycycline, among others. The tissue products noted above have also been used with disease modification in mind. None of these interventions has been shown to have a significant clinical benefit.10 Research continues in this area, and multiple clinical trials are in progress. Another Option AmnioFix contains natural components called growth factors that have been shown to recruit the body's own stem cells to the injection site to help enhance the body's normal healing process. Growth factors are powerful agents that our bodies produce to signal cells to come to the target site, help the site to heal, and help one's own cells restore the damaged tissue. That's why for many years these tissues have been believed to be potentially useful in treating patients with cartilage damage and OA. AmnioFix Injectable, MiMedx Group, Inc's micronized dehydrated human amnion/chorion membrane, is a tissue derived from donated placentas that possesses anti-inflammatory properties, displays low immunogenicity, and promotes healing. AmnioFix is the product of a manufacturing process in which amniotic tissues donated by mothers having planned C-sections and screened for infectious microorganisms undergo the PURION process, in which bioactive components are retained despite the tissue being revitalized, dehydrated, and sterilized. This tissue contains multiple important growth factors believed to be important for healing in the setting of OA. AmnioFix has been shown to recruit mesenchymal stem cells to the site of injection.11 Multiple scientific studies support the potential of AmnioFix to have beneficial effects on cartilage when seeded with chondrocytes.12 AmnioFix does not contain live stem cells and is not categorized as a stem cell injection. AmnioFix, available as an injection administered by a physician, is a new option to enhance healing and modulate inflammation in various injuries and clinical conditions. Amniotic membrane, including AmnioFix, has been the subject of many scientific publications evaluating its use in wound care, orthopedics, sports medicine, and a multitude of other surgical applications. Primarily, it's been shown to be safe and effective in this setting. Interesting scientific data from nonhuman studies tend to support this potential. For example, the Willett and Guldberg et al study, referenced previously, underscores the potential for AmnioFix to preserve cartilage in the setting of joint trauma.4 In a rat model of OA (surgical damage to a knee joint structure, the meniscus, induces OA in rats), the researchers' experiments demonstrated that micronized dehydrated amniotic membrane is "rapidly sequestered in the synovial membrane (the membrane lining the joint) following intra-articular injection and attenuates cartilage degradation. … These data suggest that intra-articular delivery of micronized dehydrated amniotic membrane may have a therapeutic effect on OA development." The authors note that the ease of injection and the fact that the material is retained in the joint space are important attributes favoring use in this setting. They also note and report low immunogenicity and the promotion of wound healing. This hopeful work is continuing with further experimentation in collaboration with scientists in the US military. Clinical results from a well-controlled human study in plantar fasciitis also support the potential safety and efficacy of injectable micronized dehydrated amniotic membrane in another traumatic and common rheumatologic condition. In this study, this product was successfully used to treat the painful inflammatory and debilitating condition plantar fasciitis.13 This condition is believed to be caused by repetitive trauma and, like OA, is characterized by pain and disability that may become chronic. The trial was randomized and blinded and results showed that injection was safe and produced marked reduction in pain scores, improved quality of life, and improved ankle scores. Only minimal site injection symptoms, mainly limited pain and swelling, were observed in a minority of patients. A second successful study in this indication has recently been completed and is in the process of publication. In addition, substantial interest has been generated for use in injecting traumatic sites, including sports injuries, bursitis, Achilles tendonitis, and other related clinical problems. The safety profile of the product in these setting has been remarkably benign to date. AmnioFix may be a nonsteroidal option if conservative treatments such as anti-inflammatories, physical therapy, and bracing have not provided symptomatic relief, and may help people stay active longer and postpone or even prevent surgery. Reimbursement varies by payer, and patients are encouraged to talk to their doctors about any out-of-pocket costs. In Practice We are in the process of publishing the results of our first 100 patients to have six-month follow-ups postinjection for knee OA. In our electronic medical record, we routinely enter important clinical data, including pain scores and the Knee Injury and Osteoarthritis Outcome Score (KOOS), for all patients. To date, our results have been encouraging and have provided the framework for ongoing placebo-controlled clinical trials. The KOOS evaluation tool measures pain and important functions like ability to perform daily activities. The initial results of these observations can be seen in Figure 2.
Noteworthy is that all scales improved from baseline, some more than others. Importantly, sports and recreation and quality of life measures showed impressive improvement from values taken before injection. My patients have been generally satisfied with their results. Many will have mild-moderate pain after injection, lasting up to a several days. As we have observed, symptomatic clinical improvement starts within the first few weeks and continues over the six-month observation period. Typical comments are similar to those of my patient, Laura, a 78-year-old. Laura has had both her shoulder and her knee injected with AmnioFix. She says, "I had the AmnioFix injection, and within four weeks I was moving quite a bit better and within six weeks it seemed the pain was gone. I had no more pain. I may be 78, but I'm very active, and I just need that quality of life. I couldn't have been more pleased because I'm back to my crafts and my quality of life is back to normal again." Laura hopes that "more information gets out and that more people see that it's working and that it's not invasive," and notes, "it doesn't take time away from your life, your quality of life returns much sooner, and just because you're older doesn't mean you don't want a quality of life." Laura comments, "My mother lived to be 96 and I want to at least beat her record. So I may have a few more injections of the AmnioFix before I'm done." Many of my patients have had similar responses. Some will require surgery at a point in time but see AmnioFix, as do I, as a potential way to at least put surgery off to the future. In summary, knee OA is a very common, costly, and debilitating problem for older adults. Most treatments to date have largely targeted symptomaticity, but there is much interest in regenerative medicine approaches to treatment in patients that have not responded adequately to these usual standard measures. AmnioFix appears to be an intervention that potentially provides great value in relieving symptoms and improving quality of life in the many patients affected by OA. Early evidence suggests that there's hope that the response to its use is durable and may provide longer lasting regenerative benefits. This product is an important tool in our practice for the care of these patients and we are continuing to work diligently to fully explore its overall value and place in our treatment regimens. — Kris Alden, MD, PhD, is a fellowship-trained, board-certified orthopaedic surgeon. He specializes in hip, knee, and shoulder reconstruction, and is a leader in the field of joint replacement. Alden practices with a multidisciplinary orthopaedic group, Hinsdale Orthopaedics, and draws patients from all over the Midwest and across the United States. He was awarded the Kate and Michael Barany Award for research and scholarship and also received the Outstanding PhD Thesis award for his biophysics research on calcium channel function in skeletal and cardiac muscle and neuron functioning. His graduate work was published in multiple scientific journals. As a practicing surgeon, Alden has lectured on and trained other surgeons in novel primary and complex joint reconstruction techniques across North America and Europe. References 2. Guccione AA, Felson DT, Anderson JJ, et al. The effects of specific medical conditions on the functional limitations of elders in the Framingham Study. Am J Public Health. 1994;84(3):351-358. 3. Barbour KE, Stevens JA, Helmick CG, et al. Falls and fall injuries among adults with arthritis—United States, 2012. MMWR Morb Mortal Wkly Rep. 2014;63(17):379-383. 4. Willet NJ, Thote T, Lin AS, et al. Intra-articular injection of micronized dehydrated human amnion/chorion membrane attenuates osteoarthritis development. Arthritis Res Ther. 2014;16(1):R47. 5. Cutler DM, Ghosh K. The potential for cost savings through bundled episode payments. N Engl J Med. 2012;366(12):1075-1077. 6. Deshpande B, Katz JN, Solomon DH, Yelin EH, Losina E. Burden of symptomatic knee osteoarthritis in the United States: impact of race/ethnicity, age and sex. Paper presented at: ACR/ARHP Annual Meeting; November 9, 2015; San Francisco, CA. 7. Xie F, Kovic B, Jin X, He X, Wang M, Silvestre C. Economic and humanistic burden of osteoarthritis: a systematic review of large sample studies. Pharmacoeconomics. 2016;34(11):1087-1100. 8. Hunter DJ, Schofield D, Callander E. The individual and socioeconomic impact of osteoarthritis. Nat Rev Rheumatol. 2014;10(7):437-441. 9. Fang M, Noiseux N, Linson E, Cram P. The effect of advancing age on total joint replacement outcomes. Geriatr Orthop Surg Rehabil. 2015;6(3):173-179. 10. Martel-Pelletier J, Wildi LM, Pelletier JP. Future therapeutics for osteoarthritis. Bone. 2012;51(2):297-311. 11. Maan ZN, Rennert RC, Koob TJ, Januszyk M, Li WW, Gurtner GC. Cell recruitment by amnion chorion grafts promotes neovascularization. J Surg Res. 2015;193(2):953-962. 12. Lei J, Priddy LB, Lim JJ, Massee M, Koob TJ. Identification of extracellular matrix components and biological factors in micronized dehydrated human amnion/chorion membrane. Adv Wound Care (New Rochelle). 2017;6(2):43-53. 13. Zelen CM, Poka A, Andrews J. Prospective, randomized, blinded, comparative study of injectable micronized dehydrated amniotic/chorionic membrane allograft for plantar fasciitis—a feasibility study. Foot Ankle Int. 2013;34(10):1332-1339. |