January/February 2018
Oral Health: Essential Element of Healthful Aging Members of geriatrics care teams must launch a renewed focus on maintaining healthy mouths in older adults, not only for their physical health and self-image but also for the downstream cost savings associated with diseases related to poor oral health. "… I have never encountered patients who said they were comfortable if their mouths were uncomfortable. Think about it. The time is long overdue to include good oral health in our core definition of what it means to be truly healthy. Working together, we can identify and implement the best way to make quality oral health care accessible to older adults who need it." As people in the United States and many other countries around the world enjoy longer, fuller lives, improving and maintaining oral health is increasingly recognized as more than a lofty goal. A healthy mouth is an integral and necessary part of a whole-person approach to health care as delivered by an interprofessional team that combines the efforts of all of those caring for older adults—primary care and specialty physicians, nurses, nurse practitioners, pharmacists, social workers, psychologists, physical and occupational therapists, care partners and family members, and dental professionals as well. Whether it's through direct care, education, or information, we all have a role to play. Why is oral health so important? Without a healthy mouth, important aspects of general and health-related quality of life are affected, including nutrition, self-image, social interactions, mental health, and, all too often, physical health. The connections between oral health and systemic health are clear and very important. Over the past year and a half, I have been privileged to lead a workgroup established by The Gerontological Society of America (GSA) that is spreading the word about ways of enhancing and maintaining oral health in older adults with the goal of better quality of life and improved health outcomes. We welcome this opportunity to share some of the highlights of our recent GSA publications, conferences, and presentations about geriatric oral health.2,3 The Mouth-Body Connection This connection between the mouth and the body points to the need to remove historical barriers between medicine and dentistry. An example of the old paradigm of practice is illustrated by the acronym HEENT, the standard shorthand medical professionals use when referring to examination of the head, eyes, ears, nose, and throat. We agree with those who have advocated that HEENT should be transformed to HEENOT, by including the oral cavity as part of a thorough physical examination in all settings.16 Since oral disease is now associated with systemic conditions such as diabetes, respiratory conditions, and endocarditis, why would any health professional ignore the mouth during routine physical examinations? Dental caries is essentially a bacterial infection on the surfaces of the teeth, and periodontal disease is caused by effects of pathogenic bacteria on gums and supporting structures. The bacteria responsible for both of these conditions originate in dental plaque that regularly accumulates in the mouth and must be removed to prevent oral disease. Along with producing oral disease, oral infections are now recognized as leading to the introduction of bacteria into the respiratory tract and bloodstream, potentially leading to serious systemic health problems. Diabetes is perhaps the "prototype" condition that illustrates the bidirectional and interrelated nature of oral health and systemic disease.17 Patients with poorly controlled diabetes have a threefold greater risk of developing gingivitis and periodontal disease, and those with diabetes whose periodontal disease is treated have improved metabolic control of diabetes, fewer complications, and improved quality of life.18 Tooth loss is greater among adults with diabetes than among those without the disease.19 Other systemic conditions linked to poor oral health and/or periodontal disease include the following: • Case control and cohort studies have shown a clear relationship between various respiratory disorders and poor oral health and hygiene. Bacteria from plaque in the mouth can be transported into the respiratory tract and there produce aspiration pneumonia or complicate conditions such as COPD.20 • Patients taking certain medications for treating osteoporosis are at risk for osteonecrosis, a rare but serious complication that can occur after intraoral trauma from infections, injuries, or extractions exposes the jaw bones to oral bacteria. Osteonecrosis is associated with use of bisphosphonates and denosumab, which are also used in patients with bone cancer.21,22 • Xerostomia (dry mouth) complicates oral health on many levels, from promoting tooth decay to impairing functions such as speaking, tasting, chewing, and swallowing. Polypharmacy and use of medications on the Beers list (particularly several agents that cause dry mouth) should be avoided in older adults.23,24 • The high doses of radiation used in treatment of head and neck cancer can produce a permanent decrease in salivary output and an altered consistency of saliva, leading to problems with oral health. Combined with difficulty swallowing and mucosal sensitivity that develop as late symptoms and other related soft tissue problems (mucositis, candidiasis, mouth pain, and orofacial neuropathic pain), these cancer survivors often make alterations to their diets to avoid pain and sensitivity, leading to malnutrition that has been associated with functional deficits and overall decline.25 • There also continues to be great interest in possible relationships between oral health and atherosclerotic cardiovascular disease. While ischemic heart disease and ischemic stroke have been associated with periodontal disease in some case control or cohort studies, this link may be related to the general inflammation in blood vessels that each of these conditions can produce.26,27 • Another intriguing area of research is the potential relationship between oral health and cognitive impairment. While some studies suggest that people with good oral hygiene habits and who are seen regularly by dentists have lower risks for cognitive decline and onset of dementia, cognitive impairment could be leading to poor oral health, rather than the other way around.28 On the positive side, studies suggest that individuals with dementia can maintain their dentition just as well as those without dementia when comprehensive dental care is provided.29-31 Creating Interprofessional Oral Health Champions in Everyday Practice
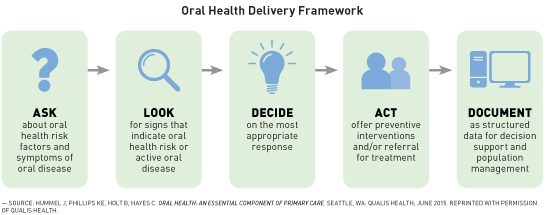
• Ask about symptoms that suggest oral disease and factors that place patients at increased risk for oral disease. Two or three simple questions can be asked to elicit symptoms of oral dryness, pain or bleeding in the mouth, oral hygiene and dietary habits, and length of time since the patient last saw a dentist. These questions can be asked verbally or included in a written health risk assessment. • Look for signs that indicate oral health risk or active oral disease. Assess the adequacy of salivary flow; look for signs of poor oral hygiene, white spots or cavities, gum inflammation, recession, or loose teeth; and examine the oral mucosa and tongue for signs of disease. • Decide on the most appropriate response. Review information gathered and share results with patients and families. Determine a course of action using standardized criteria based on the answers to the screening and risk assessment questions; findings of the oral exam, and the values, preferences, and goals of the patient and family. • Act by delivering preventive interventions and/or placing an order for a referral to a dentist or medical specialist. Preventive interventions delivered in the primary care setting may include changes in the medication list to protect the saliva, teeth, and gums; fluoride therapy; dietary counseling to protect the teeth and gums and to promote glycemic control for patients with diabetes; oral hygiene training; and therapy for tobacco, alcohol, or drug addiction. Refer to dental professionals. • Document the findings as structured data to organize information for decision support, measure care processes, and monitor clinical outcomes so that quality of care can be managed. General advice about daily oral hygiene can be delivered by all health professionals using points such as those in the preventive care sidebar, below. Our GSA workgroup believes that outreach to other health professions should begin during the educational process. A number of initiatives are under way in this arena. Thanks to the efforts of the Interprofessional Education Collaborative,33 health professional students of all types can rotate through dental offices and other oral health settings. For practicing professionals, continuing education programs can increase knowledge about oral health for physicians, nurses, pharmacists, and other health professionals.34 Smiles for Life (www.smilesforlifeoralhealth.org) has produced educational resources to promote the integration of oral health and primary care. The intended result is the development of more interprofessional champions who connect with each other and with patients to help improve oral health, especially in underserved rural and low-income areas, culturally diverse communities, and long term care where access to comprehensive oral health services can be especially problematic. Achieving Medicare Coverage for Oral Health Services Several organizations are now working together to expand dental insurance options for older adults and push for creation of a national oral health benefit under Medicare. The benefit is badly needed by those whose quality of life and overall health will be compromised by poor oral health as a result of a lack of professional care. Despite the challenges of expanding Medicare coverage, including basic oral health services makes a lot of sense. Aside from the clear relationships between oral and systemic health previously described, there is growing evidence that downstream medical costs for conditions such as diabetes and aspiration pneumonia can be reduced with improved oral health care.36,37 The Santa Fe Group is one of the organizations advocating for an oral health benefit under Medicare by working with governmental partners, health professional associations, nonprofit foundations, and insurance companies.37 Our GSA workgroup is also involved in this effort, as are Oral Health America and the American Dental Association.2,3,38 Until there is more broadly available dental coverage for older adults, other potential resources for dental care for those without insurance or with limited income include federally qualified health centers or other community clinics that may offer dental services on a sliding-fee basis, as well as clinics at local dental or dental hygiene schools. State and county dental societies usually maintain lists of low-cost dental clinics and those accepting Medicaid, as well as any free clinics that may be available in the community. Focusing on the Future Through a Coalition of Oral Health Champions Through our Oral Health Workgroup, GSA is seeking to empower everyone involved in elder care by maximizing the interprofessional efforts of dozens of partnering organizations, and to identify and publicize champions for oral health in older adults. We are establishing an online comprehensive compilation of resources that allows users to link to relevant information scattered across the internet and to communicate and share information. Clinicians and educators can now more easily connect with others to support their activities, while researchers in the aging field who are interested in expanding into oral health now have a way to connect with oral health experts for guidance on funding, study design, and methodology. Coalition members will also serve as mentors for young academicians, researchers, and clinicians interested in pursuing specialization in oral health within their fields. Through these efforts, we hope to ensure that all Americans can age more gracefully, enjoying all the advantages that improved oral health affords through better nutrition, communication, socialization, and overall health. We all have a role to play in making oral health a greater priority in older adults. — Stephen Shuman, DDS, MS, is chair of the Oral Health Workgroup of The Gerontological Society of America and an associate professor and director of the Oral Health Services for Older Adults Program at the University of Minnesota School of Dentistry and Graduate School. * On behalf of The Gerontological Society of America's Oral Health Workgroup Acknowledgments: This article is based on workgroup publications prepared by Shuman and other members of the oral health workgroup, as follows: Xi Chen, DDS, PhD, is an associate professor in the department of preventive and community dentistry at the University of Iowa College of Dentistry and Dental Clinics; Paula K. Friedman, DDS, MSD, MPH, is an emeritus professor, former director of the section on geriatrics and gerontology, and former director of the Geriatric Dentistry Fellowship at Boston University Henry M. Goldman School of Dental Medicine; Elisa M. Ghezzi, DDS, PhD, is an adjunct clinical assistant professor at the University of Michigan School of Dentistry; Michèle J. Saunders, DMD, MS, MPH, is an adjunct professor in the department of psychiatry at the University of Texas Health Science Center; and Bei Wu, PhD, is Dean's Chair Professor in Global Health at New York University Rory Meyers College of Nursing. Also acknowledged are The Gerontological Society of America for continued support, GlaxoSmithKline Consumer Healthcare for grant support, and L. Michael Posey, BSPharm, MA, for editorial support. References 2. Shuman S, Chen X, Friedman PK, Ghezzi EM, Saunders MJ, Wu B; The Gerontological Society of America. Oral health: an essential element of healthy aging. https://www.geron.org/images/gsa/documents/oralhealth.pdf. Published 2017. 3. The Gerontological Society of America. Interprofessional solutions for improving oral health in older adults: addressing access barriers, creating oral health champions. https://www.geron.org/images/gsa/documents/gsa2017oralhealthwhitepaper.pdf. Published July 2017. 4. McClearn GE, Svartengren M, Pedersen NL, Heller DA, Plomin R. Genetic and environmental influences on pulmonary function in aging Swedish twins. J Gerontol. 1994;49(6):264-268. 5. Lee KH, Wu B, Plassman BL. Cognitive function and oral health-related quality of life in older adults. J Am Geriatr Soc. 2013;61(9):1602-1607. 6. Park H, Suk S-H, Cheong J-S, et al. Tooth loss may predict poor cognitive function in community-dwelling adults without dementia or stroke: the PRESENT project. J Korean Med Sci. 2013;28(10):1518-1521. 7. Del Brutto OH, Gardener H, Del Brutto VJ, et al. Edentulism associates with worse cognitive performance in community-dwelling elders in rural Ecuador: results of the Atahualpa project. J Community Health. 2014;39(6):1097-1100. 8. Lee KH, Plassman BL, Pan W, Wu B. Mediation effect of oral hygiene on the relationship between cognitive function and oral health in older adults. J Gerontol Nurs. 2016;42(5):30-37. 9. Han P, Sun D, Yang J. Interaction between periodontitis and liver diseases. Biomed Rep. 2016;5(3):267-276. 10. Joshy G, Arora M, Korda RJ, Chalmers J, Banks E. Is poor oral health a risk marker for incident cardiovascular disease hospitalisation and all-cause mortality? Findings from 172,630 participants from the prospective 45 and Up Study. BMJ Open. 2016;6(8):e012386. 11. Ruokonen H, Nylund K, Furuholm J, et al. Oral health and mortality in patients with chronic kidney disease. J Periodontol. 2017;88(1):26-33. 12. Beukers NG, van der Heijden GJ, van Wijk AJ, Loos BG. Periodontitis is an independent risk indicator for atherosclerotic cardiovascular diseases among 60,174 participants in a large dental school in the Netherlands. J Epidemiol Community Health. 2017;71(1):37-42. 13. Friedman PK, Lamster IB. Tooth loss as a predictor of shortened longevity: exploring the hypothesis. Periodontol 2000. 2016;72(1):142-52. 14. Padilha DM, Hilgert JB, Hugo FN, Bós AJ, Ferrucci L. Number of teeth and mortality risk in the Baltimore Longitudinal Study of Aging. J Gerontol A Biol Sci Med Sci. 2008;63(7):739-744. 15. Zhang W, Wu YY, Wu B. Does oral health predict functional status in late life? Findings from a national sample [published online March 1, 2017]. J Aging Health. doi: 10.1177/0898264317698552. 16. Haber J, Hartnett E, Allen K, et al. Putting the mouth back in the head: HEENT to HEENOT. Am J Public Health. 2015;105(3):437-441. 17. Li S, Williams PL, Douglass CW. Development of a clinical guideline to predict undiagnosed diabetes in dental patients. J Am Dent Assoc. 2011;142(1):28-37. 18. Dolan TA, Berkey D. Planning for the future. In: Friedman PK, ed. Geriatric Dentistry: Caring for Our Aging Population. Ames, IA: John Wiley & Sons; 2014:303. 19. American Dental Association. For the dental patient: diabetes: tips for good oral health. http://www.ada.org/en/~/media/ADA/Publications/Files/For_the_Dental_Patient_July_2010. Published July 2010. Accessed October 26, 2017. 20. Olsen I. From the acta prize lecture 2014: the periodontal-systemic connection seen from a microbiological standpoint. Acta Odontol Scand. 2015;73(8):563-568. 21. Rollason V, Laverrière A, MacDonald LC, Walsh T, Tramèr MR, Vogt-Ferrier NB. Interventions for treating bisphosphonate-related osteonecrosis of the jaw (BRONJ). Cochrane Libr. 2016;2:CD008455. 22. Dodson TB. The frequency of medication-related osteonecrosis of the jaw and its associated risk factors. Oral Maxillofac Surg Clin North Am. 2015;27(4):509-516. 23. Skaar DD, O'Conner H. Using the Beers criteria to identify potentially inappropriate medication use by older adult dental patients. J Am Dent Assoc. 2017;148(5):298-307. 24. American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 updated Beers criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2015;63(11):2227-2246. 25. Murphy BA, Deng J. Advances in supportive care for late effects of head and neck cancer. J Clin Oncol. 2015;33(29):3314-3321. 26. "New" periodontal disease and cardiovascular disease. American Diabetes Association website. http://www.ada.org/en/science-research/science-in-the-news/new-periodontal-disease-and-cardiovascular-disease. Published October 21, 2015. Accessed October 26, 2017. 27. Bale BF, Doneen AL, Vigerust DJ. High-risk periodontal pathogens contribute to the pathogenesis of atherosclerosis. Postgrad Med J. 2017;93(1098):215-220. 28. Li J, Hanzhang X, Pan W, Wu B. Association between tooth loss and cognitive decline: a 13-year longitudinal study of Chinese older adults. PLoS One. 2017;12(2):e0171404. 29. Chen X, Shuman SK, Hodges JS, Gatewood LCC, Xu J. Patterns of tooth loss in older adults with and without dementia: a retrospective study based on a Minnesota cohort. J Am Geriatr Soc. 2010;58(12):2300-2307. 30. Dental care every day: a caregiver's guide. National Institute of Dental and Craniofacial Research website. http://www.nidcr.nih.gov/OralHealth/Topics/DevelopmentalDisabilities/DentalCareEveryDay.htm. Published February 2012. Accessed October 26, 2017. 31. Wu B, Fillenbaum GG, Plassman BL, Guo L. Association between oral health and cognitive status: a systematic review. J Am Geriatr Soc. 2016;64(4):739-751. 32. Hummel J, Phillips KE, Holt B, Hayes C. Oral health: an essential component of primary care. http://www.safetynetmedicalhome.org/sites/default/files/White-Paper-Oral-Health-Primary-Care.pdf. Published June 2015. Accessed October 26, 2017. 33. Interprofessional Education Collaborative. Core competencies for interprofessional collaborative practice: 2016 update. https://www.tamhsc.edu/ipe/research/ipec-2016-core-competencies.pdf. Published 2016. 34. Spolarich A. Training pharmacists to counsel older adults about oral health. Paper presented at: International Association for Dental Research General Session; March 24, 2017; San Francisco, CA. 35. Yarbrough C, Nasseh K, Vujicic M; Health Policy Institute, American Dental Association. Why adults forgo dental care: evidence from a new national survey. http://www.ada.org/~/media/ADA/Science%20and%20Research/HPI/Files/HPIBrief_1114_1.ashx. Published November 2014. Accessed October 26, 2017. 36. Jeffcoat MK, Jeffcoat RL, Gladowski PA, Bramson JB, Blum JJ. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-174. 37. Slavkin HC; Santa Fe Group. A national imperative: oral health services in Medicare. J Am Dent Assoc. 2017;148(5):281-283. 38. Our legislative priorities. Oral Health America website. https://oralhealthamerica.org/about/legislative-priorities. Accessed October 26, 2017.
RESOURCES • Love the Gums You're With: Patient resources on the American Academy of Periodontology website (www.perio.org/consumer/patient-resources) and the organization's GUMBLR website for "all things gums" (http://loveyourgums.tumblr.com) • Mouth Care Without a Battle: An evidence-based approach to person-centered daily mouth care for individuals with cognitive and physical impairment (www.mouthcarewithoutabattle.org) • Mouth Healthy: Consumer-facing website of the American Dental Association (www.mouthhealthy.org) • Oral Health: Federal resources listed on the Health Resources and Services Administration website (www.hrsa.gov/oral-health/index.html) • Smiles for Life: Resources useful for professionals teaching students in the health professions or interacting directly with patients about oral health (www.smilesforlifeoralhealth.org) • Tooth Wisdom: Health resources developed by the nonprofit Oral Health America for older adults regarding the importance of oral health, finding dental care services, and paying for care (www.toothwisdom.org)
PREVENTIVE ORAL CARE IN OLDER ADULTS Older adults and their families need to know that good dental care does not have to be complicated or expensive. Those without dental coverage can seek reduced-cost or free professional care at federally qualified health centers, dental schools, or providers who accept Medicaid. For daily hygiene, the only requirements are manual dexterity (or assistance from a family member or aide) and a toothbrush, toothpaste, dental floss, mouth rinse and, if needed, cleansers and brushes for dentures. Manual toothbrushes are inexpensive and effective when used properly two or more times daily. The older person or a caregiver helping with oral hygiene should select a toothbrush with a handle, head, and bristles of appropriate shape and size. Older people often have limited dexterity. For them, powered toothbrushes can greatly assist with oral hygiene. The longer handles are easier to grasp, and greater effectiveness of the rapidly rotating head enables older people to keep their teeth, tongue, and gums cleaner and healthier. A basic fluoride toothpaste is all most people need. Older adults whose teeth are sensitive because of gum recession, caries (cavities), or other factors or with xerostomia (dry mouth) can select one of several specially formulated toothpastes. Dental floss and/or other interdental cleaning devices should be used daily to remove plaque between the teeth and thereby prevent inflammation and caries. Patient preference is generally the most important consideration in choosing a dental floss (waxed/unwaxed, flavors, thickness of strands), and other interdental cleaning devices (eg, floss handles, interdental brushes) can make things easier for those who cannot floss with their fingers. Older people, especially those who have sensitive teeth and/or xerostomia, generally prefer mouth rinses that are fluoridated and alcohol-free. Rinses with higher fluoride concentrations are available by prescription. Removable dentures need the same cleaning regularity as natural teeth but with different products. Minimally abrasive denture cleaners or mild soap and water should be applied with a denture brush twice daily, after which the dentures can be soaked in an appropriate marketed solution. The wearer should rinse the dentures using water or a nonalcoholic antimicrobial mouth rinse and also rinse the mouth with that type of product before reinserting the dentures. |